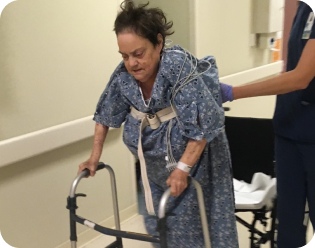
This 74 yr female was reffered to me for incerasing breathing difficulty and b/l pedal edema, loss of apettite and frequent diarrhea (4-5 /day) since last 6 month .
She is known as a case of hypertension ( 5yrs-on ARB), hypothyroidism ( well controlled on 100mcg) since last 5 years
She was evaluated for these ailments -HRCT AND CTPA- NORMAL. ECHO TR with RA /RV DILATED ( PASP 54)
OTHER ROUTINE BLOOD REPORTS NORMAL.
SHE IS ON ECOSPRIN, CLOPIDOGREL, AND ROSUVASTATIN AS WELL.
NO SIGNS OF BRONCHOSPASM.
B/L TENSE NON-PITTING EDEMA
B/L PLEURAL EFFUSION -TAPPING -TRANSUDATE .
LAST 15 DAYS HER URINE OUTPUT IC DECREASED TO LESS THAN 400ML
SHE IS HAVING DIARRHEA AT LEAST 5-6 TIMES.
After a careful history and examination what I found that Hypertension and hypothyroidism were detected almost together, edema was non-pitting, she has blackish tongue & cheek discoloration, breathing difficulty seems to be more related to chronic fluid overload rather pulmonary or cardiac. Tachycardia was due high Eltroxin dose ( 100mcg- TSH <0.03 MCG/DL). As rule of thumb whenever I see hypothyroidism associated hypoadrenalism I would like to rule out. Relative hypoadrenalism get worse if Eltroxin is given without steroid replacement. Other clues were tongue pigmentation, relative low Na(128) and high K 4.5( despite on diuretics, explained abdominal pain and diarrhea. I asked for anti-microsomal / thyroid antibody (>1200) which was high, ACTH 58(23-48) high, 6 am cortisol 18 ( should have been above 30 in view of high ACTH. Short -SYN ACTH test confirmed relative adrenaline insufficiency.
Telmisartan has a tendency to affect renal perfusion -so it was stopped. amlodipine causes pedal edema so it was stopped.
Tab Hydrocortisone 40 mg started and Eltroxin reduced to 88.5 mcg. In three days time, she lost 4 kg weight, breathing difficulty reduced by >60%, diarrhea stopped. A surprising finding is that she does not need antihypertensive now.
Dx – autoimmune thyroiditis, relative adrenaline insufficiency with secondary hypertension.